Chinese Journal of Tissue Engineering Research ›› 2013, Vol. 17 ›› Issue (46): 8018-8023.doi: 10.3969/j.issn.2095-4344.2013.46.007
Previous Articles Next Articles
Effect of hyperbaric oxygen preconditioning on expression of Bcl-2 and Bax after spinal cord injury
Zhang Yu-qiang1, Li You2, Cao Yang1, Dong Ming-yan1, Lü Gang1
- 1 Department of Orthopedics, 2 Department of Ophthalmology, the First Affiliated Hospital of Liaoning Medical University, Jinzhou 121000, Liaoning Province, China
-
Online:2013-11-12Published:2013-11-30 -
About author:Zhang Yu-qiang☆, M.D., Department of Orthopedics, the First Affiliated Hospital of Liaoning Medical University, Jinzhou 121000, Liaoning Province, China zhangyuqiang1981@163.com
CLC Number:
Cite this article
Zhang Yu-qiang, Li You, Cao Yang, Dong Ming-yan, Lü Gang. Effect of hyperbaric oxygen preconditioning on expression of Bcl-2 and Bax after spinal cord injury[J]. Chinese Journal of Tissue Engineering Research, 2013, 17(46): 8018-8023.
share this article
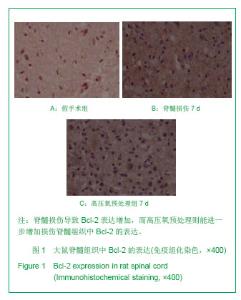
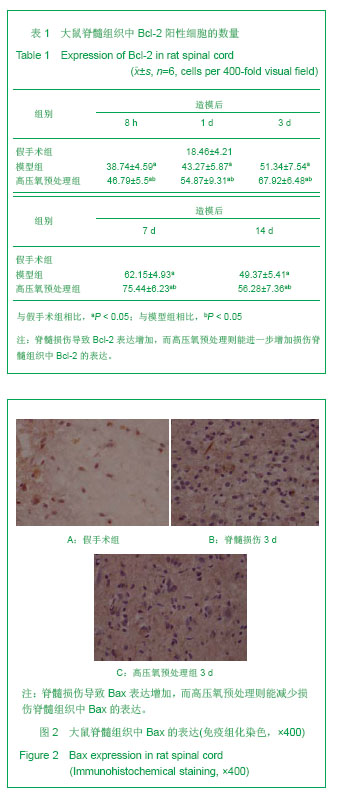
2.1 实验动物数量分析 纳入SD大鼠66只,其中7只大鼠因术后感染死亡,并进行了补充,在进入结果分析时无脱失。 2.2 高压氧预处理对大鼠损伤脊髓中Bcl-2表达的影响 免疫组化染色显示,Bcl-2阳性表达的特征为神经元和胶质细胞胞浆或/和胞膜见棕黄色颗粒。假手术组脊髓组织中可见少量Bcl-2阳性细胞,见图1A。模型组脊髓灰质和白质中均可见Bcl-2阳性细胞,脊髓损伤8 h仅有少量Bcl-2阳性细胞,损伤第1天时Bcl-2阳性细胞开始增多,损伤第3天Bcl-2阳性细胞数进一步增加,损伤第7天达高峰,损伤后第14天仍可见大量Bcl-2阳性细胞,见图1B。高压氧预处理组脊髓灰质和白质均表达Bcl-2,表达高峰亦出现在伤后第7天,但高压氧预处理组大鼠脊髓中Bcl-2阳性细胞数量均显著高于模型组(P < 0.05),见图1C,表1。"
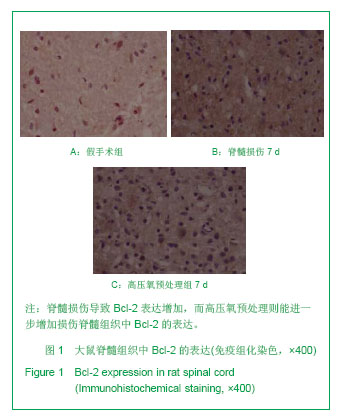
| [1]王晓红,邵彬,王琴,等.高压氧治疗对脊髓损伤后大鼠神经细胞凋亡及行为学评分的影响[J].重庆医学,2010,39(8):935-936. [2]谷莉娜,郑杨,王奭骥,等.高压氧预处理对正常和糖尿病大鼠缺血再灌注心肌细胞凋亡的影响[J].中国老年学杂志,2011,31(11): 3306-3308. [3]蔡宏斌,葛朝明,赵翀翀,等. 不同压力高压氧预处理与大鼠脑缺血灌注损伤缺血半暗带神经元细胞凋亡[J].中国康复医学杂志,2011,26(1): 50-54. [4]张铨,陈明华,吴俊山,等.高压氧预处理对兔脊髓缺血再灌注损伤的保护机制探讨[J].现代生物医学进展,2010,10(21): 4049- 4051. [5]徐帆,陈建敏,张晓.脊髓损伤动物模型的制备及神经功能评价[J].创伤外科杂志,2007,9(1):91-93. [6]Fan DF, Liu K, Xu WG, et al. Hyperbaric oxygen preconditioning reduces the incidence of decompression sickness in rats via nitric oxide. Undersea Hyperb Med. 2010; 37(3):173-180. [7]Yogaratnam JZ, Laden G, Guvendik L, et al. Pharmacological preconditioning with hyperbaric oxygen: can this therapy attenuate myocardial ischemic reperfusion injury and induce myocardial protection via nitric oxide? J Surg Res. 2008; 149(1):155-164. [8]Gempp E, Blatteau JE. Preconditioning methods and mechanisms for preventing the risk of decompression sickness in scuba divers: a review. Res Sports Med. 2010; 18(3):205-218. [9]Lu PG, Hu SL, Hu R, et al. Functional recovery in rat spinal cord injury induced by hyperbaric oxygen preconditioning. Neurol Res. 2012;34(10):944-951. [10]Tai PA, Chang CK, Niu KC, et al. Attenuating experimental spinal cord injury by hyperbaric oxygen: stimulating production of vasculoendothelial and glial cell line-derived neurotrophic growth factors and interleukin-10. J Neurotrauma. 2010;27(6):1121-1127. [11]Huang L, Mehta MP, Nanda A, et al. The role of multiple hyperbaric oxygenation in expanding therapeutic windows after acute spinal cord injury in rats. J Neurosurg. 2003;99(2 Suppl):198-205. [12]Cheng O, Ostrowski RP, Wu B, et al. Cyclooxygenase-2 mediates hyperbaric oxygen preconditioning in the rat model of transient global cerebral ischemia. Stroke. 2011;42(2): 484-490. [13]Liu M, Wu XP, Tong M. Effect of ultra-early hyperbaric oxygenation on spinal edema and hind limb motor function in rats with complete spinal cord transection. Nan Fang Yi Ke Da Xue Xue Bao. 2009;29(10):2014-2017. [14]He X, Xu X, Fan M, et al. Preconditioning with hyperbaric oxygen induces tolerance against renal ischemia-reperfusion injury via increased expression of heme oxygenase-1. J Surg Res. 2011;170(2):e271-277. [15]Li WC, Jiang DM, Hu N, et al. Lipopolysaccharide preconditioning attenuates neuroapoptosis and improves functional recovery through activation of Nrf2 in traumatic spinal cord injury rats. Int J Neurosci. 2013;123(4): 240-247. [16]Yan W, Zhang H, Bai X, et al. Autophagy activation is involved in neuroprotection induced by hyperbaric oxygen preconditioning against focal cerebral ischemia in rats. Brain Res. 2011;1402:109-121. [17]Ok JH, Kim YH, Ha KY. Neuroprotective effects of hypothermia after spinal cord injury in rats: comparative study between epidural hypothermia and systemic hypothermia. Spine (Phila Pa 1976). 2012;37(25):E1551-1559. [18]Yin X, Meng F, Wang Y, et al. Effect of hyperbaric oxygen on neurological recovery of neonatal rats following hypoxic-ischemic brain damage and its underlying mechanism. Int J Clin Exp Pathol. 2013;6(1):66-75. [19]Peng Y, Feng SF, Wang Q, et al. Hyperbaric oxygen preconditioning ameliorates anxiety-like behavior and cognitive impairments via upregulation of thioredoxin reductases in stressed rats. Prog Neuropsychopharmacol Biol Psychiatry. 2010;34(6):1018-1025. [20]Ostrowski RP, Graupner G, Titova E, et al. The hyperbaric oxygen preconditioning-induced brain protection is mediated by a reduction of early apoptosis after transient global cerebral ischemia. Neurobiol Dis. 2008;29(1): 1-13. [21]Liu Y, Sun XJ, Liu J, et al. Heme oxygenase-1 could mediate the protective effects of hyperbaric oxygen preconditioning against hepatic ischemia-reperfusion injury in rats. Clin Exp Pharmacol Physiol. 2011;38(10):675-682. [22]Liu KJ, Xu J, Yang CY, et al. Analysis of olfactory ensheathing glia transplantation-induced repair of spinal cord injury by electrophysiological, behavioral, and histochemical methods in rats. J Mol Neurosci. 2010;41(1):25-29. [23]Maybhate A, Hu C, Bazley FA, et al. Potential long-term benefits of acute hypothermia after spinal cord injury: assessments with somatosensory-evoked potentials. Crit Care Med. 2012;40(2):573-579. [24]Hu R, Zhou J, Luo C, et al. Glial scar and neuroregeneration: histological, functional, and magnetic resonance imaging analysis in chronic spinal cord injury. J Neurosurg Spine. 2010; 13(2):169-180. [25]Han X, Yang N, Xu Y, et al. Simvastatin treatment improves functional recovery after experimental spinal cord injury by upregulating the expression of BDNF and GDNF. Neurosci Lett. 2011;487(3):255-259. [26]Xiong L, Zhu Z, Dong H, et al. Hyperbaric oxygen preconditioning induces neuroprotection against ischemia in transient not permanent middle cerebral artery occlusion rat model. Chin Med J (Engl). 2000;113(9):836-839. [27]Contreras IS, Moreira LF, Ballester G, et al. Immediate ischemic preconditioning based on somatosensory evoked potentials seems to prevent spinal cord injury following descending thoracic aorta cross-clamping. Eur J Cardiothorac Surg. 2005;28(2):274-279. [28]Lee JS, Yang CC, Kuo YM, et al. Delayed granulocyte colony-stimulating factor treatment promotes functional recovery in rats with severe contusive spinal cord injury. Spine (Phila Pa 1976). 2012;37(1):10-17. [29]Amemori T, Jendelová P, R?zicková K, et al. Co-transplantation of olfactory ensheathing glia and mesenchymal stromal cells does not have synergistic effects after spinal cord injury in the rat. Cytotherapy. 2010;12(2): 212-225. [30]Colak A, Antar V, Karao?lan A, et al. Q-VD-OPh, a pancaspase inhibitor, reduces trauma-induced apoptosis and improves the recovery of hind-limb function in rats after spinal cord injury. Neurocirugia (Astur). 2009;20(6):533-540. [31]All AH, Bazley FA, Gupta S, et al. Human embryonic stem cell-derived oligodendrocyte progenitors aid in functional recovery of sensory pathways following contusive spinal cord injury. PLoS One. 2012;7(10):e47645. [32]Colak A, Karao?lan A, Barut S, et al. Neuroprotection and functional recovery after application of the caspase-9 inhibitor z-LEHD-fmk in a rat model of traumatic spinal cord injury. J Neurosurg Spine. 2005;2(3):327-334. [33]Zhang YP, Burke DA, Shields LB, et al. Spinal cord contusion based on precise vertebral stabilization and tissue displacement measured by combined assessment to discriminate small functional differences. J Neurotrauma. 2008;25(10):1227-1240. [34]Jadhav V, Ostrowski RP, Tong W, et al. Hyperbaric oxygen preconditioning reduces postoperative brain edema and improves neurological outcomes after surgical brain injury. Acta Neurochir Suppl. 2010;106:217-220. [35]Guo X, Bu X, Li Z, et al. Comparison of autologous bone marrow mononuclear cells transplantation and mobilization by granulocyte colony-stimulating factor in experimental spinal injury. Int J Neurosci. 2012;122(12):723-733. [36]Yune TY, Kim SJ, Lee SM, et al. Systemic administration of 17beta-estradiol reduces apoptotic cell death and improves functional recovery following traumatic spinal cord injury in rats. J Neurotrauma. 2004;21(3):293-306. [37]Kubota K, Saiwai H, Kumamaru H, et al. Myeloperoxidase exacerbates secondary injury by generating highly reactive oxygen species and mediating neutrophil recruitment in experimental spinal cord injury. Spine (Phila Pa 1976). 2012; 37(16):1363-1369. [38]Onifer SM, Nunn CD, Decker JA, et al. Loss and spontaneous recovery of forelimb evoked potentials in both the adult rat cuneate nucleus and somatosensory cortex following contusive cervical spinal cord injury. Exp Neurol. 2007;207(2): 238-247. [39]Martinez M, Brezun JM, Zennou-Azogui Y, et al. Sensorimotor training promotes functional recovery and somatosensory cortical map reactivation following cervical spinal cord injury. Eur J Neurosci. 2009;30(12):2356-2367. [40]Yu CG, Jimenez O, Marcillo AE, et al. Beneficial effects of modest systemic hypothermia on locomotor function and histopathological damage following contusion-induced spinal cord injury in rats. J Neurosurg. 2000;93(1 Suppl):85-93. [41]Chen HC, Fong TH, Hsu PW, et al. Multifaceted effects of rapamycin on functional recovery after spinal cord injury in rats through autophagy promotion, anti-inflammation, and neuroprotection. J Surg Res. 2013;179(1):e203-210. [42]Zeng Y, Xie K, Dong H, et al. Hyperbaric oxygen preconditioning protects cortical neurons against oxygen-glucose deprivation injury: role of peroxisome proliferator-activated receptor-gamma. Brain Res. 2012; 1452:140-150. [43]Hillard VH, Peng H, Das K, et al. Inhibition of x-irradiation-enhanced locomotor recovery after spinal cord injury by hyperbaric oxygen or the antioxidant nitroxide tempol. J Neurosurg Spine. 2007;6(4):337-343. [44]Han X, Yang N, Cui Y, et al. Simvastatin mobilizes bone marrow stromal cells migrating to injured areas and promotes functional recovery after spinal cord injury in the rat. Neurosci Lett. 2012;521(2):136-141. [45]Wang YC, Zhang S, Du TY, et al. Hyperbaric oxygen preconditioning reduces ischemia-reperfusion injury by stimulating autophagy in neurocyte. Brain Res. 2010;1323: 149-151. [46]Yan W, Zhang H, Bai X, et al. Autophagy activation is involved in neuroprotection induced by hyperbaric oxygen preconditioning against focal cerebral ischemia in rats. Brain Res. 2011;1402:109-121. [47]Zeng Y, Xie K, Dong H, et al. Hyperbaric oxygen preconditioning protects cortical neurons against oxygen-glucose deprivation injury: role of peroxisome proliferator-activated receptor-gamma. Brain Res. 2012;1452: 140-150. [48]卢培刚,冯华,胡荣,等.高压氧预处理对脊髓损伤后轴突再生影响实验研究[J].中华神经外科疾病研究杂志, 2011,11(4):316-320. [49]李洪鹏,巴方,白丹,等.高压氧预处理对脊髓损伤后后角神经元的保护作用[J].中国医科大学学报,2012,41(1):11-13. [50]Li JS, Zhang W, Kang ZM, et al. Hyperbaric oxygen preconditioning reduces ischemia-reperfusion injury by inhibition of apoptosis via mitochondrial pathway in rat brain. Neuroscience. 2009;159(4):1309-1315. [51]Wang L, Li W, Kang Z, et al. Hyperbaric oxygen preconditioning attenuates early apoptosis after spinal cord ischemia in rats. J Neurotrauma. 2009;26(1):55-66. |
| [1] | Wen Dandan, Li Qiang, Shen Caiqi, Ji Zhe, Jin Peisheng. Nocardia rubra cell wall skeleton for extemal use improves the viability of adipogenic mesenchymal stem cells and promotes diabetes wound repair [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1038-1044. |
| [2] | Zhang Yujie, Yang Jiandong, Cai Jun, Zhu Shoulei, Tian Yuan. Mechanism by which allicin inhibits proliferation and promotes apoptosis of rat vascular endothelial cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1080-1084. |
| [3] | Deng Shuang, Pu Rui, Chen Ziyang, Zhang Jianchao, Yuan Lingyan . Effects of exercise preconditioning on myocardial protection and apoptosis in a mouse model of myocardial remodeling due to early stress overload [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(5): 717-723. |
| [4] | Li Anan, Jiang Tao, Zhan Min, Cai Yuning, Song Min, Li Congcong, Lin Wenzheng, Zhang Jiayuan, Liu Wengang. Pharmacological mechanism of Shenling Baizhu San in the treatment of knee osteoarthritis based on network pharmacology and molecular docking [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(2): 197-204. |
| [5] | Wei Wenyue, Wang Yuyin, Guo Minfang, Zhang Jing, Gu Qingfang, Song Lijuan, Chai Zhi, Yu Jiezhong, Ma Cungen. Fasudil inhibits neuronal apoptosis via regulating mitochondrial dynamics in APP/PS1 mice [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(2): 232-238. |
| [6] | Yu Dong, Liu Kan, Shi Zongting, Yang Xiaoxia, Liu Hengping, Zhang Qingfeng. Pathological changes of the cervical intervertebral discs and rules of migration and apoptosis in endplate chondrocytes in a rabbit model of dynamic disequilibrium [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(11): 1675-1679. |
| [7] | Xing Hongchang, Cao Jianping, Zhu Jing, Yao Kun. Mechanism by which enalapril alleviates myocardial injury in a rat model of limb ischemia-reperfusion [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(11): 1747-1751. |
| [8] | Cai Shengsheng, Mei Heng, Zhang Xuequan, Deng Jin, Cao Jun, He Bin. Prepared HPe6DF composite nanoparticles enhance the effect of photodynamic therapy [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(10): 1566-1573. |
| [9] | Meng Defeng, Li Changzai, Wu Chuntao. Effects of LINC02532 targeting miR-145 on proliferation, migration, invasion and apoptosis of pancreatic cancer stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(1): 52-58. |
| [10] | Yao Yanyi, Chen Xiaoling, Zhang Min, Wang Hong, Hao Liying, Shi Chao, Zhao Bingfeng, Jin Yaqiao, Dong Wei. miR-210/YWHAG axis with adipocyte proliferation and angiogenesis after autologous fat transplantation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(1): 59-63. |
| [11] | Li Zhongkang, Zheng Jiahua, Tian Yanpeng, Huang Xianghua. Latest progress and mechanisms of mesenchymal stem cells on premature ovarian failure [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(1): 141-147. |
| [12] | Li Jing, Xie Jianshan, Cui Huilin, Cao Ximei, Yang Yanping, Li Hairong. Expression and localization of diacylglycerol kinase zeta and protein kinase C beta II in mouse back skin with different coat colors [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1196-1200. |
| [13] | Geng Qiudong, Ge Haiya, Wang Heming, Li Nan. Role and mechanism of Guilu Erxianjiao in treatment of osteoarthritis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1229-1236. |
| [14] | Pei Lili, Sun Guicai, Wang Di. Salvianolic acid B inhibits oxidative damage of bone marrow mesenchymal stem cells and promotes differentiation into cardiomyocytes [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1032-1036. |
| [15] | Li Shibin, Lai Yu, Zhou Yi, Liao Jianzhao, Zhang Xiaoyun, Zhang Xuan. Pathogenesis of hormonal osteonecrosis of the femoral head and the target effect of related signaling pathways [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 935-941. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||